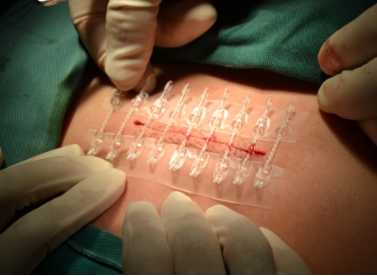
Tissue adhesive, also known as tissue glue or surgical adhesive, is a medical adhesive used to bond tissues together in various medical and surgical procedures. It adheres to biological tissue to form a safe and sterile closure or bond without the need for sutures or staples. Tissue adhesives are typically made from biocompatible materials. They are commonly used in medical and healthcare settings for wound closure, tissue repair and other medical procedures.
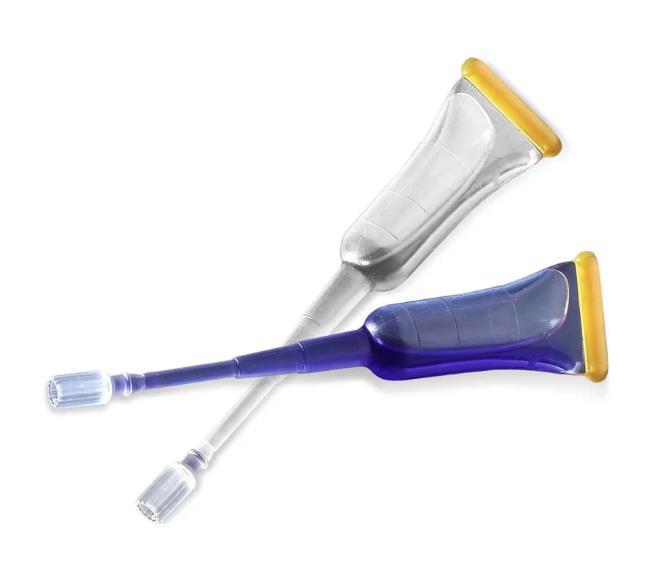
The main components of tissue adhesives typically include cyanoacrylate compounds that polymerize (harden) when exposed to moisture, thereby forming a strong bond between the tissues to which they are attached. Tissue adhesives are sterile and come in disposable applicators or vials to ensure aseptic application. Below is information about their uses, benefits, and how they are applied:
1. Uses:
- Wound Closure: Tissue adhesive is commonly used to close small incisions, lacerations, or surgical incisions rather than traditional sutures or skin staples. It is particularly useful for wound closure in areas that may be difficult or unsightly, such as the face or scalp.
- Dermatology: Dermatologists use tissue adhesives for minor skin procedures such as mole removal or skin biopsies.
- Dentistry: In dentistry, tissue adhesives are used to bond dental restorations or as a replacement for sutures in oral surgery.
- Ophthalmology: Tissue adhesives are used in some eye surgeries to close small corneal or conjunctival incisions.
- Vascular Surgery: In some vascular surgeries, tissue adhesives are used to reinforce or seal blood vessels.
2. Advantages:
- Minimally Invasive: Tissue adhesives provide a minimally invasive option for wound closure with reduced tissue trauma compared to sutures or dermal staples.
- Aesthetically preferred: It often reduces scarring because there are no stitches or staples scars.
- Rapid application: Tissue adhesives can be applied more quickly than sutures, making them advantageous in emergency situations or for patients who are in need of rapid treatment.
- Reduced risk of infection: There is a lower risk of infection because no perforations are created that could introduce bacteria.
- No need to remove sutures: Unlike sutures, tissue adhesives do not need to be removed, reducing patient discomfort.
3. How to use tissue adhesive:
- Clean the wound: Make sure the wound is clean and dry. Remove any foreign objects or debris.
- Prepare the applicator: Tissue adhesive is usually supplied in a disposable applicator. Open the seal and prepare the applicator according to the manufacturer’s instructions.
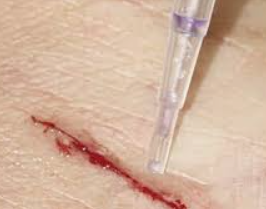
- Applying the Adhesive: Gently hold the wound edges together and apply a thin layer of tissue adhesive along the length of the wound. Avoid over-application as it slows down the drying time of the adhesive.
- Holding the Edges Together: Maintain light pressure on the wound edges for the recommended drying time, usually 30 seconds to a few minutes, depending on the specific adhesive used.
- Drying and bonding: The adhesive will bond the tissue together as it dries. Make sure the patient avoids any movement that could disrupt the bonding process during this time.
- Dressing: In some cases, a sterile dressing can be applied over the adhesive to protect the wound.
- Follow-up: Advise the patient on wound care and signs of potential infection. The tissue adhesive will fall off naturally as the wound heals.
4. Limitations of Tissue Adhesive
Although tissue adhesives offer several advantages in terms of wound closure and tissue adhesion, they have limitations and may not be appropriate in all cases. These include some of the following:
- Wound size and depth: Tissue adhesive is best for small, shallow wounds or incisions. It may not provide a strong enough closure for larger, deeper wounds or wounds under tension.
- Areas under tension: Tissue adhesives may not hold well in areas of the body where there is significant tension, such as joints or highly mobile areas. Sutures or skin staples are usually preferred in these cases. If a non-invasive skin stapler is preferred for better healing results, the BI-FIX® surgical incision closure device is a good choice.
- Contaminated wounds: Tissue adhesives may not be suitable for wounds contaminated with dirt, debris or body fluids as they require a clean and dry surface for effective adhesion. Proper wound cleansing is essential before applying tissue adhesives.
- Allergies or sensitivities: Some people may be allergic to components of tissue adhesives, such as cyanoacrylates. It is important to check for allergies or sensitivities before using on patients.
- Tissue composition: Tissue adhesives may not work equally well on all types of tissue. They may be less effective on fatty or vascularised tissue.
- Difficulty with precise alignment: Achieving precise alignment of wound edges is more challenging and difficult to fine-tune with tissue adhesives than with sutures, which allow fine-tuned control during closure.
- Embrittlement over time: Tissue adhesives become brittle over time, which can lead to reduced flexibility and, in some cases, premature bond failure.
- Lack of seal strength: Tissue adhesives may not provide the same level of tensile strength as sutures, making them less suitable for wounds subject to significant mechanical stress.
- Delayed healing: Once a tissue adhesive has been applied, it can be difficult to assess the underlying wound. With sutures, healthcare professionals can easily assess the progress of wound healing by examining the sutures.
- Cost: Tissue adhesives can be more expensive than traditional sutures, which may affect their use, especially in resource-limited settings.
5. Is new non-invasive skin closure device a good alternative to tissue adhesive?
It is important for healthcare professionals to carefully assess the patient’s wound and consider the specific situation when deciding whether to use a tissue adhesive. The choice should be based on the size, location and depth of the wound, as well as the patient’s individual needs and medical history. Given the limitations of tissue adhesives, non-invasive skin closure devices have emerged as a new class of devices that may better address the limitations of tissue adhesives in providing non-invasive closure of surgical incisions or wounds. The role of non-invasive skin closure devices versus tissue adhesives for surgical incision closure is evaluated below in several ways:
(1) Type of surgical incision:
Consider the type and complexity of the surgical incision. Non-invasive skin closure devices are usually indicated for simple, straight incisions. BI-FIX® offers better compliance than competing closure devices and can be used for all types of straight incisions, curved incisions, angled incisions and even incisions with moving parts such as joints.
(2) Tissue handling:
Assess the need for gentle tissue handling during the closure process. Non-invasive wound closure devices are designed to minimize tissue trauma, making them suitable for fragile tissues or areas of skin that require gentle treatment.
(3) Cosmetic outcomes:
Evaluate the desired cosmetic outcome of the surgical incision. Both non-invasive skin closure devices and tissue adhesives can provide good cosmetic results, but the choice may depend on the surgeon’s preference and expertise, as well as the specifics of the incision. For small incisions, both tissue adhesives and non-invasive skin closure devices can provide cosmetic results, and for larger, more tense incisions, non-invasive skin closure devices are more appropriate to avoid suture puncture scars.
(4) Speed and efficiency:
Consider the efficiency of the closure method. Non-invasive closure devices can provide rapid epidermal closure. This can be an advantage in procedures where time is of the essence. Tissue adhesives are also well known for their ability to be applied quickly.
(5) Risk of infection:
Assess the risk of infection associated with each method. Both non-invasive skin closure devices and tissue adhesives aim to minimize the risk of infection by providing secure wound closure without perforating the skin. When tissue adhesives are used, the wound is more closed and may have a higher risk of infection than non-invasive closure devices if there is exudate that cannot be drained.
(6) Expertise of the surgical team:
Assess the experience and training of the surgical team. At present, new non-invasive skin closure devices may require specialized training for proper use, whereas the use of tissue adhesives is usually already familiar to many healthcare professionals.
(7) Availability of resources:
Consider the availability of resources and materials in the surgical environment. Some non-invasive devices may be more expensive than tissue adhesives, which may affect their use, and this should be considered in terms of affordability in the local market.
(8) Patient comfort and rehabilitation:
Consider patient comfort and post-operative recovery. Both aim to minimize patient discomfort and promote faster recovery.
(9) Incision tension:
Assess whether there will be significant tension at the incision site. Surgical techniques such as suturing or stapling may be preferable to non-invasive incision closure devices or tissue adhesives in cases of high tension. If a skin closure device such as the BI-FIX® is to be used on a high-tension wound, consider reducing the tension with sutures first and then using the BI-FIX® for skin tension reduction, resulting in better wound healing.
(10) Surgeon preference:
Consider the surgeon’s preference and familiarity with each wound closure method. Surgeons may have personal preferences based on their experience and expertise. When promoting a new product, it is important to give the surgeon confidence to try the new product with professional skills and provide good instruction and training in its use.
บทสรุป
In conclusion, the choice of a non-invasive skin closure device or tissue adhesive for closure of a surgical incision should be based on a comprehensive evaluation of the specific surgical procedure, the type of incision, the surgeon’s experience and the patient’s needs. Both methods can play an important role in surgical wound closure and decisions may vary depending on individual circumstances and clinical preferences. Collaborative decision-making by the surgical team is essential to ensure the best patient outcome.